A survey published this month by National Nurses United (NNU) depicted the stark reality of workplace violence (WPV) among healthcare workers. The survey focused on the increase in violent incidents based on data gathered from 2023.
The report shines a light on safety concerns healthcare workers are facing in hospitals, outpatient clinics, and other facilities. In the survey, 81.6 percent of nurses said they had experienced WPV in 2023. Of the 991 nurses surveyed, 3 in 10 reported they’ve been physically harmed at work, including being slapped, punched, or scratched.¹
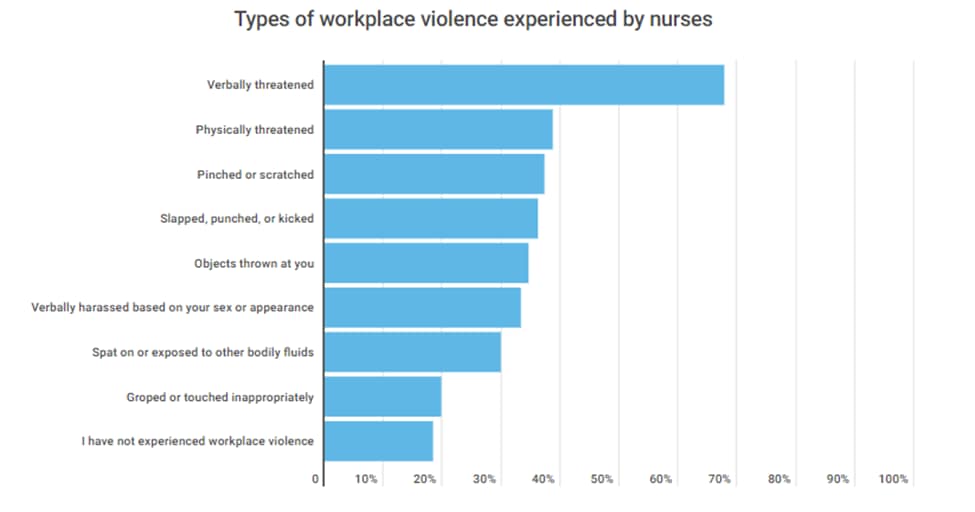
[Graph from https://www.advisory.com/daily-briefing/2024/02/08/nnu-survey]
These numbers have climbed drastically in recent years, with over 45 percent of nurses reporting an increase in violence in their workplace in the past twelve months¹—a number that was already up 119 percent from 2021 to 2022.²
A nurse from Kentucky shared some of her recent experiences: “In the past year I have had water pitchers, call lights, and other items thrown at me. I have been spit on, punched multiple times, and had one of my pinky fingers bent such that it seems like it will have some permanent mild pain in it that wasn’t there before.”
But the violence is not only isolated to patient care areas. Many report incidents in hallways, stairwells, parking garages, and more.
A Philadelphia nurse recalled her encounter with a stranger in a parking garage: “I was coming home at 4 a.m. and the underground parking lot was mostly empty except for a few cars parked against the wall. My car was in the middle. I just about made it to my car and a guy got up from between a car and the wall and intently started walking toward me. […] He turned around and went back where he was hiding. I got in the car, locked the doors, and called security who came and got him,” she explained. “There were a bunch of reported assaulted nurses when they left work at that time. I wasn’t gonna be one.”
The Impact on Mental Health and Wellbeing
While WPV exists in other industries, data shows that healthcare workers are 5 times more likely to experience violence compared to other workers.¹ A report published in September 2022 issued by Press Ganey found that on average, two nurses are assaulted every hour.³
“Nurses take an oath to do no harm, and many put their own safety and health at risk to help a patient. However, violence should not be considered just ‘part of the job.’ What’s especially concerning about these numbers is that they are likely even higher, as assaults generally go underreported by healthcare professionals—and nurses in particular,” says Jeff Doucette, DPN, R.N., NEA-BC, FACHE, FAAN, and Chief Nursing Officer for Press Ganey.³
Nurses are expressing feelings from anxiety and fear to depression. However, only roughly a quarter of nurse respondents reported their employers provide access to counseling following violent incidents.¹ The mental anguish combined with the physical harm of WPV is pushing healthcare workers out of their jobs, contributing to the industry’s staffing shortage.
“I left the Emergency Room, the job I loved, because I wanted to be in a safe environment. I shouldn’t have to give up my passion because the system has failed us,” one Colorado nursing respondent shared.
Based on the 2023 NNU data, 19.2 percent of nurses have changed or left their jobs due to WPV, and 37.2 percent have considered leaving the profession.¹
A Need for Training and Resources
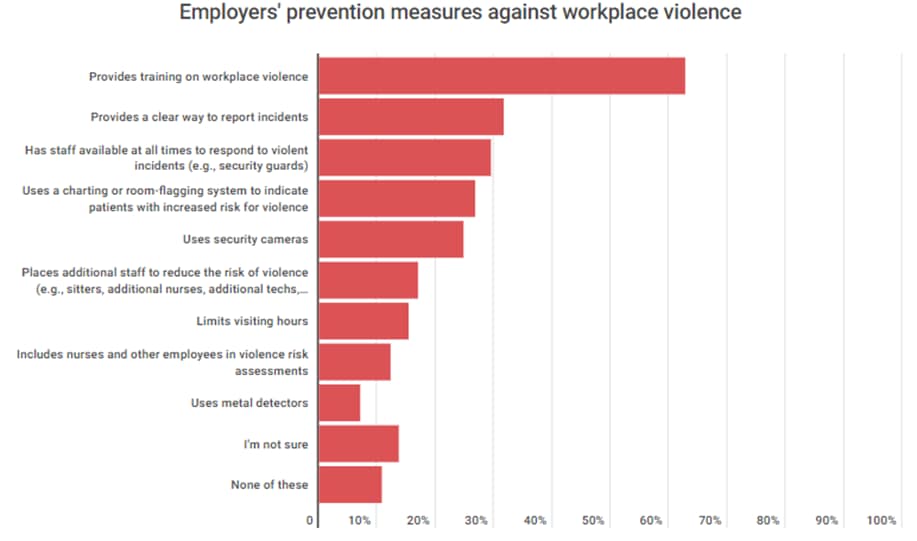
One significant finding from the NNU survey was a lack of alignment between violent incident rates and prevention measures. Despite the uptick in workplace violence among healthcare workers, we are not seeing widespread adoption of enhanced safety plans or proactive prevention measures being implemented.
[Graph from https://www.advisory.com/daily-briefing/2024/02/08/nnu-survey]
The NNU survey report states “It is unacceptable for employers to expect nurses and other health care workers to bear the brunt of workplace violence while not providing key resources and prevention measures to those employees.” But unfortunately, based on the survey results, it appears this is exactly the case.
Only about one in three nurses reported that their employer provides a clear way to report incidents; a data point critical to remedying the issue.
Nurses are also not being asked to participate in risk assessments, even though their expertise and experiences can identify the most vulnerable areas of a healthcare facility’s safety plans. This is a critical gap hindering the safety of healthcare workers today.
“When an environmental or patient-specific risk factor is identified, employers must take action to mitigate that risk factor,” the report states. “Essential workplace violence prevention measures include safe staffing, ensuring line of sight or means of immediate communication with other employees, configuring spaces so that exit routes and access to alarms cannot be blocked, removing or fastening furnishings and objects that can be improvised as weapons, preventing the transport of weapons into the facility, and maintaining an effective alarm system.”
An article published in JAMA this month also dug into this issue at hand and the progress being made to address it. The authors referenced the Legacy Good Samaritan Medical Center shooting that took place last summer in Portland, OR, and the reactive measures the facility took to strengthen safety.²
“In response to the shooting, the hospital saw the addition of metal detectors, bag searches, bullet-slowing glass, and security officers with stun guns. However, some hospital employees remain skeptical that these increased security measures will be permanently maintained in the face of the costs involved,” the authors share. They continue, summarizing legal progress being made to impact healthcare workplace violence. “State legislative actions remain critical to addressing the crisis facing health care professionals, especially considering the lack of congressional action.”²
Advocating for Policy Changes
Around the country, healthcare workers are demanding protection at a local level. In New York State, policymakers are driving a bill that would require hospitals to establish violence prevention programs and conduct annual safety and security assessments. Similar legislation passed this month in Texas, mandating that healthcare facilities must adopt workplace violence prevention policies and respond to any incidents of violence.
Mary Vitullo, BA, BSN, RN-BC, Texas Nurses Association Board Member, was an advocate pushing Texas legislation. “We had [over] 400 nurses go to the Capitol building and spoke with their representatives and senators to let them know that workplace violence is a very real part of their job right now,” she told a local news outlet last summer. “We’re facing a pretty significant nursing shortage and we need to do everything that we can to [promote eliminating things] like burnout and increasing resiliency for nurses…I think this bill is really going to help with that.”
Insights from the NNU survey amplify the need to prioritize safety for healthcare staff. Through a proactive and layered safety plan and continued policy advocacy, we can better protect the nurses and other healthcare workers who care for our communities.
CENTEGIX CrisisAlert™ empowers healthcare staff to get discreet help when and where they need it. Learn more.
¹ February 2024. HIGH AND RISING RATES OF WORKPLACE VIOLENCE AND EMPLOYER FAILURE TO IMPLEMENT EFFECTIVE PREVENTION STRATEGIES IS CONTRIBUTING TO THE STAFFING CRISIS. National Nurses United. https://www.nationalnursesunited.org/sites/default/files/nnu/documents/0224_Workplace_Violence_Report.pdf
² Ninan RJ, Cohen IG, Adashi EY. State Approaches to Stopping Violence Against Health Care Workers. JAMA. Published online February 22, 2024. doi:10.1001/jama.2024.1140
³ (2022, September 8). On average, two nurses are assaulted every hour, new Press Ganey analysis finds. Press Ganey. Retrieved February 23, 2024, from www.pressganey.com