The ability to provide high-quality care and retain employees depends upon a healthcare organization’s agility and capacity for strategic investment. In 2026, institutions are prioritizing hospital staff safety to strengthen retention, quality of care, and profitability.
Violence in healthcare has reached unprecedented levels, prompting leaders to take decisive action. The 2025 CPI Annual Workplace Violence Prevention Training Report found that healthcare organizations prioritizing safety through effective workplace violence prevention programs rose from 17 percent in 2024 to 26 percent in 2025. The following sections explore the top motivators driving these investments.
Reduced Emergency Response Time Is Critical to Hospital Staff Safety
Outdated communication platforms leave healthcare workers vulnerable during emergencies. Blue light poles, static wall panic buttons, and intercom systems fail to deliver the rapid response times that modern healthcare environments demand. These legacy systems require staff to reach a fixed location or navigate complex protocols during high-stress situations, when seconds matter.
Hospital staff safety becomes even more critical as workforce shortages increase isolation across healthcare settings. According to the National Institute for Health Care Management, the United States faces growing healthcare workforce shortages driven by maldistribution of providers, systemic factors, and rising patient demands. Thirty-one out of 35 physician specialties face ongoing shortages, and allied health, pharmacy, and nursing fields experience critical gaps.
By 2037, 47 states are projected to have a shortage of primary care physicians. Nonmetro areas will experience a 60 percent shortage of physicians, while metro areas will face a 10 percent shortage. These staffing gaps directly translate to increased isolation. Fewer colleagues on shift means fewer people nearby when a situation escalates. A nurse working alone in a remote hospital wing, a social worker conducting a late-night assessment, or a physician in an understaffed clinic all face heightened vulnerability.
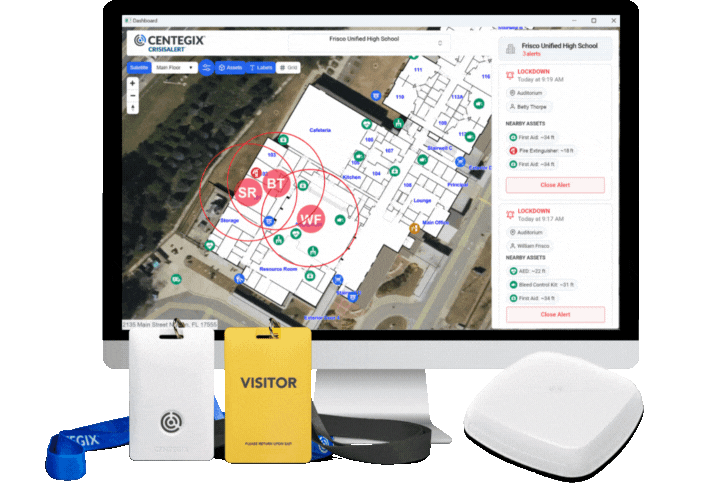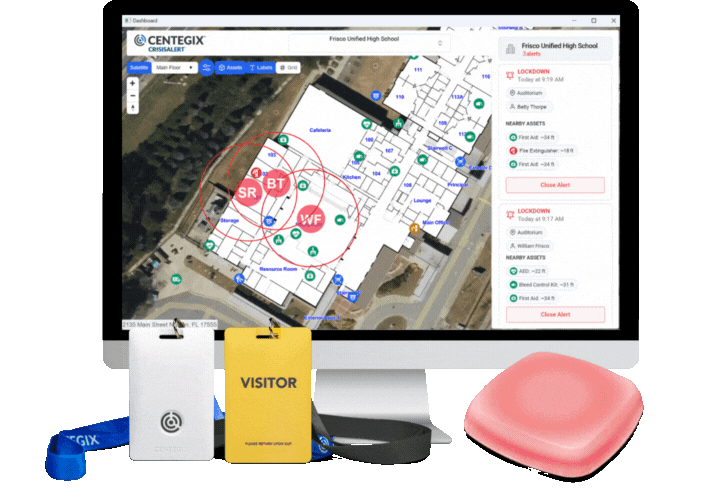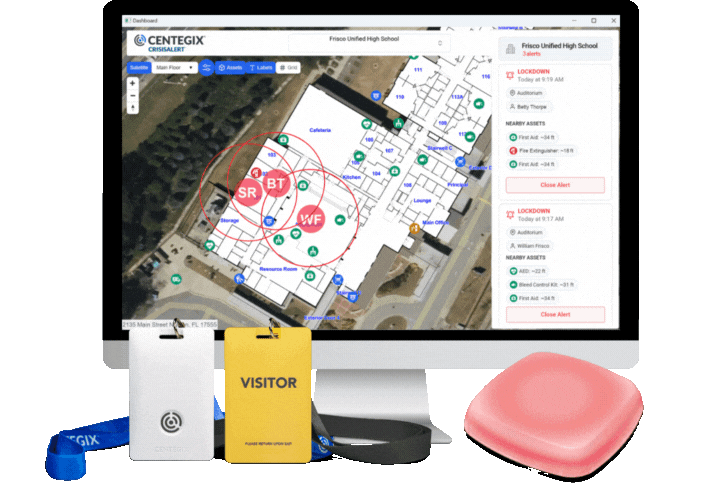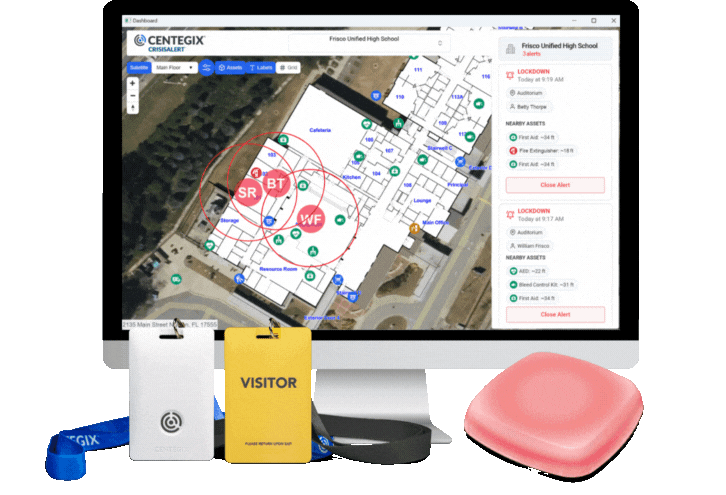
CENTEGIX® addresses this challenge through its CrisisAlert™ wearable duress button, which empowers staff to request help immediately and discreetly from anywhere on campus. The solution operates on private LoRaWAN and Bluetooth networks, eliminating dependence on Wi-Fi or cellular service. Responders receive an immediate notification with precise location information, enabling them to reduce response time and reach staff members in need.
Rising Incidents of Violence Demand Immediate Action
Recent tragedies have underscored the urgent need for comprehensive safety solutions. On Christmas Day 2025, a security guard at M Health Fairview Lakes Hospital in Wyoming, Minnesota, was killed following a confrontation with an emergency room patient. Andrea Merrell died from injuries sustained during the incident, highlighting the dangers healthcare workers face daily.
Days earlier, a social worker at Zuckerberg San Francisco General Hospital and Trauma Center was repeatedly stabbed by a patient who had allegedly threatened a doctor. Alberto Rangel, 51, died two days after the attack.
Survey data confirms these incidents reflect a broader crisis. A national survey from Black Book Research, conducted among 240 respondents including emergency department physicians, nurses, and hospital-based staff, revealed alarming findings:
- 100 percent of staff report experiencing or witnessing workplace violence, and nearly all believe current safety protocols are inadequate
- 98 percent of hospital staff support federal legislation mandating workplace violence prevention measures
- 64 percent have formally documented a violent incident
- 29 percent avoid reporting due to fear of retaliation, management inaction, or normalization of violence
The American College of Emergency Physicians found that 71 percent of survey respondents believe violence in the emergency department is worse than last year. These statistics make clear that 2026 will be a pivotal year for investing in hospital staff safety solutions.
Workforce Well-Being Directly Impacts Patient Care
Staff feel unsafe and burned out. The National Institute for Health Care Management reports that self-reported physician burnout rates remain high, with 49 percent reporting burnout and 20 percent reporting depression in 2024. Burnout is associated with an increased risk of medical errors, poor patient outcomes, and provider depression.
A growing body of research, including findings published in Public Health Reviews, highlights how chronic understaffing, compounded by poor institutional support, drives sustained stress among healthcare workers. Staff shortages increase workloads and shift lengths while eroding job satisfaction and heightening moral distress.
The American Hospital Association and CENTEGIX convened an Affinity Forum to explore the connection between safety and well-being. Panelists shared compelling data showing how workplace safety directly correlates with the patient experience.
“We know that when team members do not feel physically safe or psychologically safe in their environment, that impacts both their own well-being and the patient experience,” explained Elisa Arespacochaga, Vice President of Clinical Affairs and Workforce at the American Hospital Association. “We know that investing in safety is key to being able to employ, to improve employee engagement, their well-being, and really help overall patient care.”
Andrea Greco, Senior Vice President of Healthcare Safety at CENTEGIX, emphasized the tangible impact: “We can see not only the impact of having a safe workplace, but also protecting their mind, their body, and their talent that they direct to caring for patients. Those things combine to directly impact the perception and the feeling of patients and the level of care that they receive in those environments.”
At Vail Health Behavioral Health, the implementation of CrisisAlert duress badges has impacted retention and morale. Kim Goodrich, Behavioral Health Inpatient Operations Director, described leadership’s approach, including how they encouraged use and early adoption: “Whenever the button was pushed, there would be a little cheer from the leadership team of like, they used it. And just letting people get used to those instances of when they may or may not need it, knowing that somebody would come.”
The results speak for themselves. “It’s so far been really incredible for our retention,” Goodrich noted. “I think if we were to ask anyone at this point, they wouldn’t want us to take it away. They definitely like knowing that it’s kind of in their back pocket and a tool that they can continue to use.”
Greco reinforced the fundamental principle: “The key connection across all of that is just their ability to do the job that they have honestly sacrificed a certain amount of their time, and energy and education, and will to do, should not come with the threat of violence.”
Organizations focused on improving safety create a culture where safety is a priority for staff and patients alike. “We know that translates to a happier, more engaged workforce,” Greco added. “And when they’re feeling happier and more engaged, that allows them to perform at the highest level that they’ve been trained to do.”
Compliance with Safety Mandates Drives Investment
Legislative momentum is building at both the federal and state levels. The Workplace Violence Prevention for Health Care and Social Service Workers Act (H.R. 2531) requires healthcare employers to develop and implement workplace violence prevention plans within six months of enactment. These plans must include risk assessments, mitigation measures, incident reporting systems, and staff participation.
The Save Healthcare Workers Act (H.R. 3178/S. 1600) would make assaulting hospital staff a federal crime, with penalties of up to 10 years imprisonment for assault and enhanced penalties reaching 20 years for incidents involving weapons.
State legislation is also advancing. Ohio Governor Mike DeWine signed HB 452 into law in April 2025, requiring hospitals to establish security plans with input from multidisciplinary teams. Texas SB 240, effective September 2024, requires hospitals to create workplace violence prevention committees. Illinois is considering SB 1435, which would require hospitals to provide wearable duress buttons physically attached to employee ID badges.
The CENTEGIX Safety Platform® is an integrated safety solution that address multiple compliance needs simultaneously. Automated reporting features eliminate the burden of manual data collection and increase accessibility, while detailed dashboards display current metrics required by legislation. CrisisAlertTM duress buttons ensure that every employee can signal for help when needed.
Increasing Accountability from Employees and Unions
Employees and prospective employees demand safe workplaces and institutional support. Institutional accountability for hospital staff safety has become non-negotiable.
In early January 2026, nurses represented by the New York State Nurses Association served strike notices after contract negotiations at major private hospital systems failed to produce agreements on core workplace safety issues. Nurses and union leaders cited unsafe staffing levels, lack of adequate protections from workplace violence, and threats to healthcare benefits as major unresolved concerns.
On January 12, 2026, nearly 15,000 nurses walked off the job in what became the largest nurses’ strike in New York City history, with picket lines at multiple campuses across the city’s private hospitals.
The union’s demands have included enforceable safe staffing ratios, protections from workplace violence, and preservation of high‑quality health benefits for frontline caregivers. The action demonstrates that healthcare workers will no longer accept inadequate safety measures.
Building a Culture of Safety in Healthcare
The drivers of safety investments in 2026 converge on a single truth: healthcare organizations cannot deliver excellent patient care without first protecting their caregivers. Faster emergency response, violence mitigation, workforce well-being, regulatory compliance, and workforce accountability all point toward the same imperative.
CENTEGIX provides healthcare organizations with a comprehensive safety platform to address these challenges. The Safety Platform serves as the center of a layered safety plan, integrating wearable duress technology, dynamic digital mapping, accessible reporting, and visitor management. Healthcare leaders who invest in hospital staff safety now position their organizations for stronger retention, better patient outcomes, and compliance with emerging regulations.
Discover how CENTEGIX helps organizations exceed legislative requirements while safeguarding their workforces.